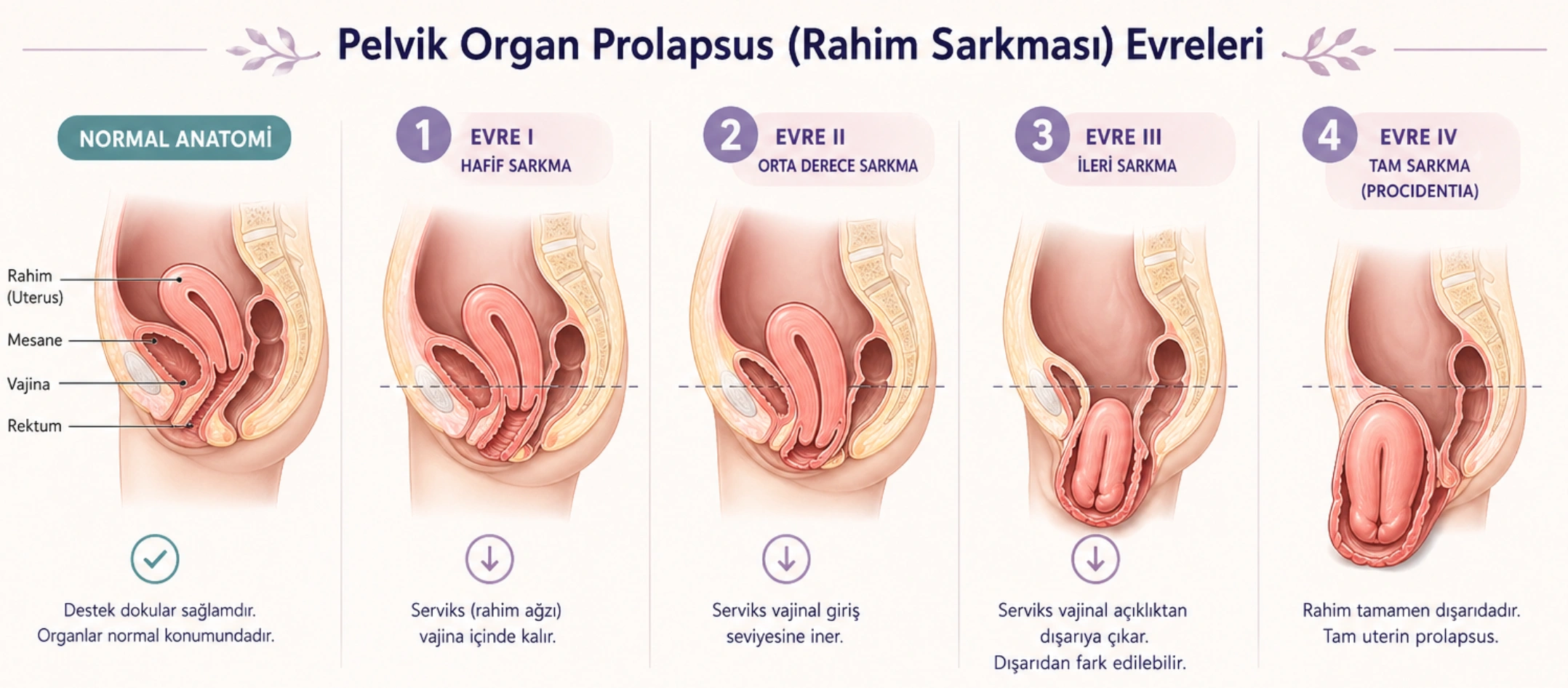
Uterine prolapse occurs when the uterus descends from its normal anatomical position due to weakening of the pelvic floor muscles and connective tissues. In advanced cases, the uterus may protrude into the vaginal canal.
The pelvic floor is a crucial support system for the uterus, bladder, and intestines. When this support structure weakens over time, prolapse may develop.
Although uterine prolapse can occur at any age, it is more commonly observed in:
• Women with a history of multiple vaginal deliveries
• Postmenopausal women
• Older age groups
Symptoms of Uterine Prolapse
Symptoms vary depending on the severity of the prolapse. Mild cases may not cause noticeable complaints, while moderate to advanced cases may present with:
• A sensation of pelvic pressure or fullness
• A feeling of downward pulling in the vagina
• Lower back or groin pain that worsens after prolonged standing
• A noticeable or palpable mass in the vagina
• Discomfort during sexual intercourse
• Urinary incontinence or difficulty urinating
• Constipation or difficulty with bowel movements
These symptoms may significantly affect quality of life.
Causes of Uterine Prolapse
Several factors may contribute to uterine prolapse:
Childbirth History
Multiple or difficult vaginal deliveries may weaken the pelvic floor.
Age and Menopause
Decreased estrogen levels may reduce connective tissue elasticity.
Obesity
Increased intra-abdominal pressure places strain on the pelvic floor.
Chronic Constipation and Straining
Persistent pressure may contribute to weakening of support structures.
Heavy Lifting
Activities that increase intra-abdominal pressure are risk factors.
Diagnosis of Uterine Prolapse
Diagnosis is typically made through a gynecological examination. During a pelvic exam, the position of the uterus and the degree of prolapse are assessed.
When necessary, additional evaluations may include:
• Pelvic ultrasound
• MRI imaging
• Urinary function tests
Treatment of Uterine Prolapse
Treatment depends on the severity of prolapse and the patient’s symptoms.
Conservative (Non-Surgical) Approaches
• Pelvic floor exercises (Kegel exercises)
• Lifestyle modifications
• Weight management
• Treatment of constipation
• Use of a pessary
A pessary is a vaginal support device that may provide symptom relief in selected patients.
Surgical Treatment
In moderate to severe cases, surgical intervention may be considered.
Surgical options include:
• Vaginal reconstructive procedures
• Laparoscopic approaches
• Uterine suspension (uterus-preserving procedures)
• Hysterectomy when medically necessary
Treatment planning is individualized based on clinical evaluation.
Recovery Process
Recovery following surgery varies depending on the technique used and individual health factors. During this period, it is important to:
• Avoid heavy lifting
• Limit activities that strain the pelvic floor
• Follow medical recommendations carefully
General Considerations
Uterine prolapse is a pelvic floor condition that may impact quality of life but can be effectively managed with appropriate care. Early evaluation allows consideration of both conservative and minimally invasive treatment options.
The decision regarding treatment should always be made individually, based on the patient’s age, expectations, and clinical condition.
FAQ
Childbirth, connective tissue weakness, and aging are the most common causes.
A feeling of vaginal fullness and downward pressure may be felt.
Yes, both surgical and non-surgical treatment options are available.
Surgery is not required in mild cases.
With proper treatment, the risk of recurrence can be reduced.