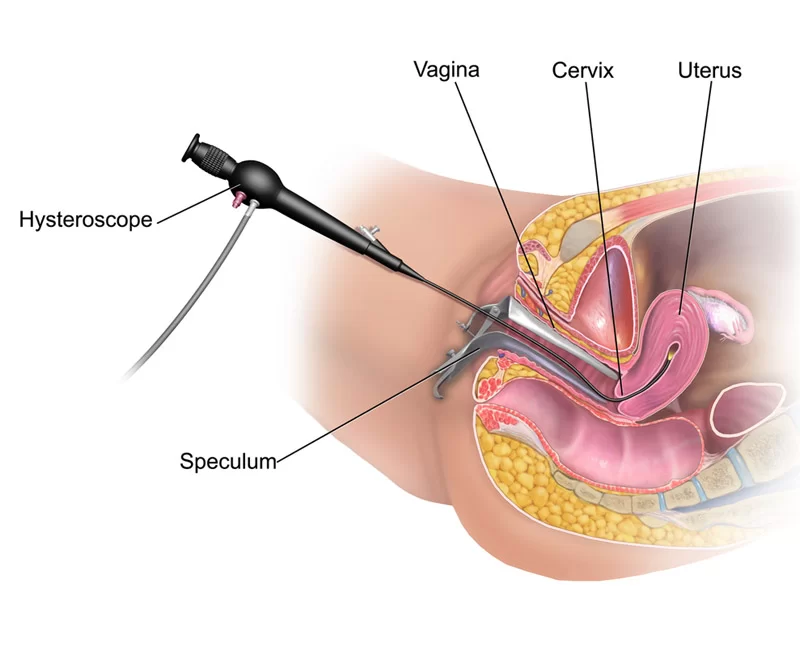
Hysteroscopy is a diagnostic and surgical gynecological procedure that allows direct visualization of the uterine cavity using a specialized imaging system. This technique is widely used for both the diagnosis and, when necessary, the treatment of intrauterine conditions.
Through hysteroscopy, the internal structure of the uterus can be examined in detail, and targeted interventions can be performed using a minimally invasive approach.
When is Hysteroscopy Performed?
Hysteroscopy may be planned for various clinical indications.
Diagnostic Hysteroscopy
• Abnormal uterine bleeding
• Suspicion of uterine polyps
• Evaluation of submucosal fibroids
• Assessment of uterine structural anomalies
• Investigation of recurrent pregnancy loss
Operative (Therapeutic) Hysteroscopy
• Removal of uterine polyps
• Removal of suitable fibroids
• Treatment of intrauterine adhesions (Asherman syndrome)
• Correction of structural abnormalities such as a uterine septum
These procedures can often be performed without the need for open surgery.
How is Hysteroscopy Performed?
Hysteroscopy is performed by gently inserting a thin optical device (hysteroscope) through the cervix into the uterus. The camera and light system attached to the hysteroscope allow direct visualization of the uterine cavity.
When necessary, surgical treatment can be performed during the same session.
The procedure is typically brief, and most patients can return to their normal activities quickly.
Advantages of Hysteroscopy
Hysteroscopy is considered a minimally invasive technique. This approach:
• Allows direct visualization of the uterine cavity
• Enables targeted treatment
• Provides a more comfortable recovery process
• May reduce the need for more extensive surgical procedures
Potential Risks and Complications
Hysteroscopy is generally a safe procedure. However, as with all medical interventions, certain risks may exist.
These may include:
• Infection
• Mild bleeding
• Rarely, uterine wall injury
• Temporary effects related to anesthesia
All aspects of the procedure are thoroughly explained prior to treatment.
General Considerations
Hysteroscopy is one of the most valuable tools in modern gynecology for evaluating and treating intrauterine conditions. The necessity of the procedure is determined based on the patient’s symptoms and clinical findings.
The most appropriate approach is always guided by an individualized physician assessment.
FAQ
It is a procedure that allows examination of the inside of the uterus using a camera.
For menstrual irregularities or suspicion of polyps or fibroids.
It is not required for diagnostic procedures but may be used for surgical ones.
It usually takes 15–30 minutes.
The same day or the following day.